Three Different Skin Disorders, Three Different Causes, Three Different Treatments
Dealing with Milia, Whiteheads, and Fungal Acne
Milia, whiteheads, and fungal acne are actually distinct disorders, each with different causes.
We all want smooth, healthy, glowing skin that keeps us looking youthful and fresh. Unfortunately, Mother Nature sometimes has other ideas, leaving us with unsightly blemishes and lumps.
This discussion centers on three skin conditions that can easily be confused because all often appear as white bumps on the skin. Milia, whiteheads, and fungal acne are actually distinct disorders, each with different causes. Knowing which one you’re dealing with is important because each requires a specific treatment response. Here’s what you need to know.
Milia Are a Type of Cyst
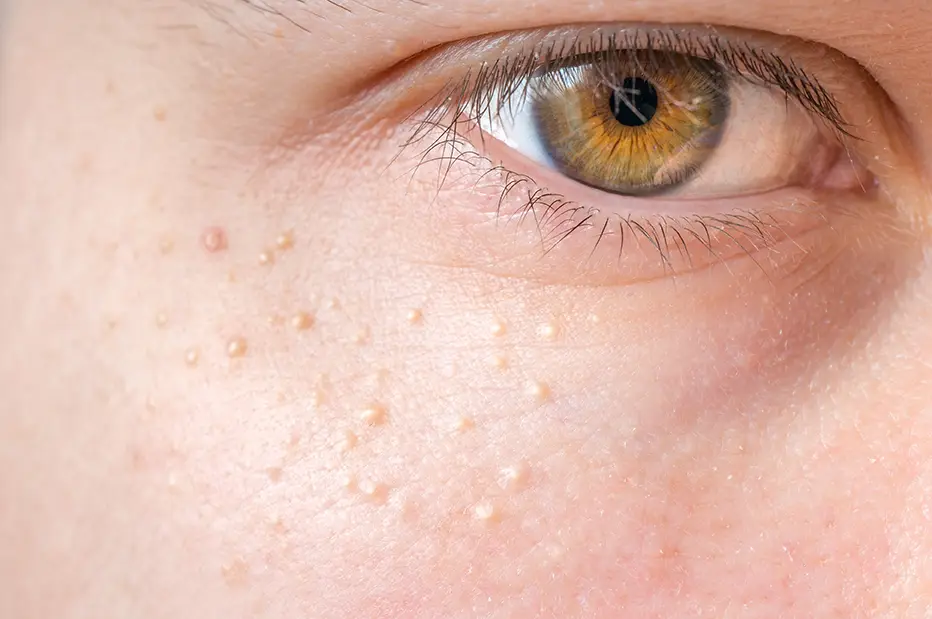
Milia are tiny white bumps that form under the outer layer of skin. Commonly found on the face, milia, which are sometimes called milk spots, are actually cysts that resemble a grain of sand or a hard, milky capsule.
A cyst is a small pocket of tissue that contains fluid, air, or another substance. In this case, that substance is old skin cells, including keratin, the protein that gives skin its structure. Milia can develop when the epidermis, your outer layer of skin, fails to shed dead cells to make room for new ones. When old skin cells don’t fall off your body, new skin grows on top of them and traps dead cells and keratin just under the surface. The old cells harden and turn into cysts. Unlike acne (they’re often confused), milia do not develop in a pore and are not red, inflamed, or painful. They’re also small, only 1 to 2 millimeters in diameter.
Most cases have no clear cause and can develop at any age, including among babies. Milia may also form after skin injuries, such as burns, sunburns, and blistering rashes, and with the use of some medications. People with acne or blackheads often have milia too, although they can appear spontaneously on clear skin as well.
How to treat milia
The best treatment is generally to do nothing. The condition is harmless and will likely clear on its own. That may take time, sometimes weeks or months. If you find milia particularly annoying, see your healthcare provider for a definitive diagnosis (there can be other causes of small, white skin bumps) and a prescription medication that helps your skin shed and replace cells faster. You can try over-the-counter products, but usually they have little effect.
Under no circumstances should you try to remove milia yourself at home. They cannot be popped or scrapped; doing so may cause scarring or infection. A healthcare professional can surgically excise milia by using a needle to puncture each spot and removing the contents with tweezers and a magnifying glass. Cryotherapy to freeze and remove spots one by one is another possibility. But the best and easiest approach is patience. Simply wait—milia will go away.
Bacteria Trapped in Pores Lead to Whiteheads
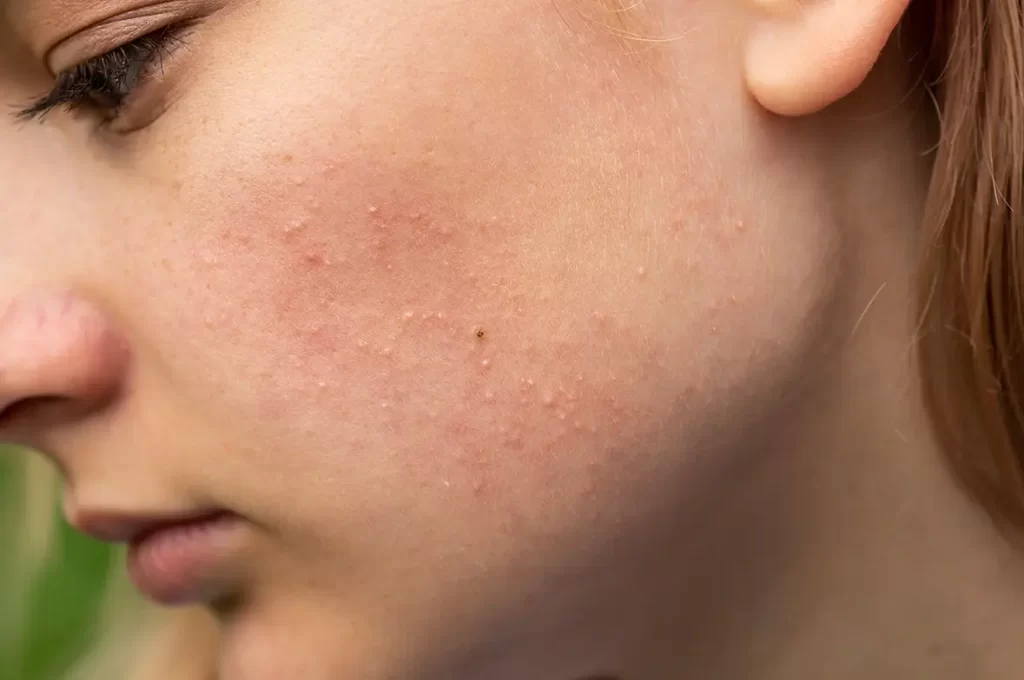
Whiteheads are a mild type of acne that displays small, closed bumps sticking up on your skin. They’re under the surface, with a white or sometimes yellowish head showing through. They develop when bacteria, dead skin, and the oily lubricant sebum (necessary for keeping your skin and hair hydrated and shiny) plug the openings of hair follicles and sebaceous (oil) glands, clogging and closing off pores. Once a pore is blocked, the debris hardens, and a white tip forms.
Also known as congested skin or a closed comedo, pimple, or zit, whiteheads are commonly found on chins, cheeks, forehead, and corners of the mouth. Adolescents and young adults are most susceptible (those pesky hormonal changes!), but blemishes can occur at any age. Dehydrated skin and using too heavy or greasy products are another cause. Blackheads are a close relative, except the pores remain open, causing dirt in the bump to appear darkened or black.
Most whiteheads disappear on their own after a week or so. They’re not contagious and rarely painful. While they don’t affect physical health, they can be a psychosocial or psychological problem, leading to anxiety, depression, mood disorders, or suicidal thoughts. Over-the-counter medications may speed treatment by removing the top layer of damaged skin and dissolving dead skin cells (salicylic acid); removing surface bacteria (benzoyl peroxide); or breaking up whiteheads (and blackheads) by minimizing the oil production that causes clogged pores (retinols and retinoids). Many brand-name products are available at numerous price points; reading labels carefully lets you know which items offer what benefits so you can decide what’s right for you.
Treatment for whiteheads
For serious cases, your healthcare provider can assist with prescription-strength retinoids or oral antibiotics. Physical removal of whiteheads is possible using microdermabrasion to sand off top layers of skin to free clogged pores; chemical peels to remove layers of skin; or laser skin resurfacing with pulsating beams of light that reduces the amount of oil your sebaceous glands produce. Such measures are for professional use only and should never be attempted on your own. Even squeezing or popping whiteheads is not advisable. Applying pressure can push bacteria deep into cells causing inflammation or producing scarring by damaging your skin.
Mostly, try not to worry. Whiteheads are harmless and will clear up on their own.
With Fungal Acne, the Name Says It All
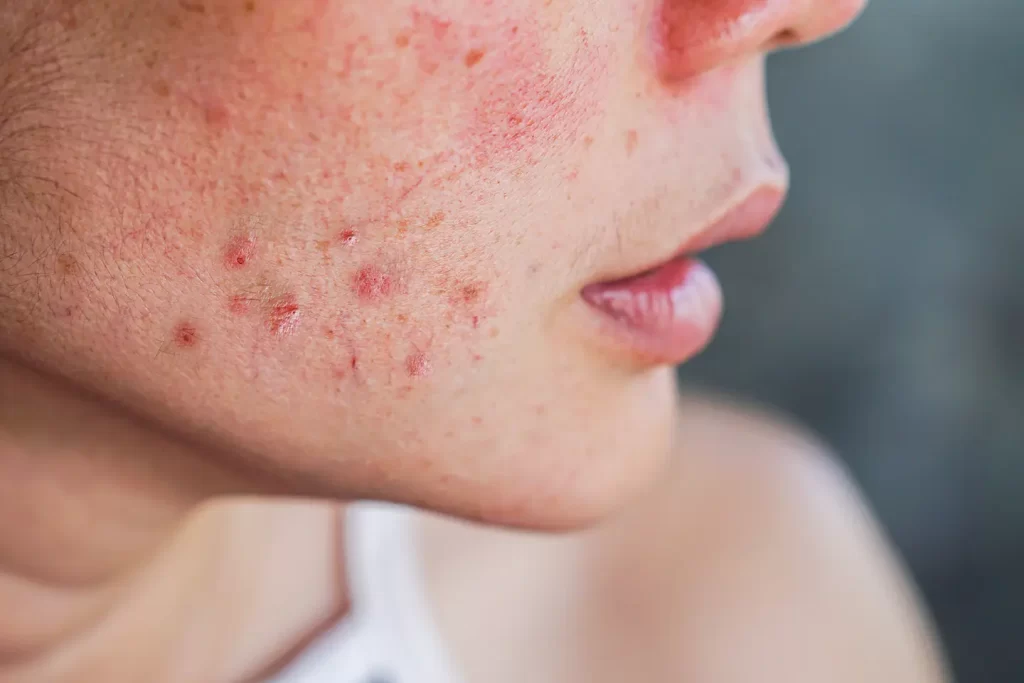
Malassezia folliculitis, the scientific name for fungal acne, refers to an infection in the hair follicles. Fungal acne is different from common acne (like whiteheads, which develop when follicles get blocked with bacteria, oil, and dead skin) because it’s caused by the fungus Malassezia, a type of yeast naturally found on everyone’s skin. This yeast can get inside hair follicles and grow, causing the follicle to react by becoming inflamed; the resulting infection generates pockets of white pustules or red bumps that show up in rash-like clusters on the forehead, chin, neck, chest, or back. These eruptions tend to be sudden and itchy or burning, which is a clue that you’re dealing with fungal acne rather than common acne or some other painless skin disorder.
Who will get fungal acne?
Although anyone can get fungal acne, it’s most common among adolescents and young adult males; they tend to have the oily skin yeast needs to thrive. The condition is most likely in those who live in hot, humid climates; sweat a lot or have naturally greasy skin; wear tight-fitting clothing, especially while exercising; suffer from other fungal infections, a weakened immune system; or use antibiotics. Coating the skin with heavy, oil-based moisturizers and sunscreens can also be a culprit, as the skin can skin be damaged by excessive rubbing, shaving, plucking, or touching that traps yeast in hair follicles, giving it a place to grow.
If you suspect fungal acne, get a diagnosis
Fungal acne is best diagnosed by a dermatologist or other healthcare professional. They may scrape a spot and examine the sample under a microscope to see if yeast spores are present. Treatment involves prescribing oral or topical antifungal medications, creams, and shampoos. Antibiotics don’t help. In extreme cases that don’t respond well to other treatments, photodynamic therapy combining light and a drug may be used to destroy unhealthy fungal cells. The disorder can recur, so working with your healthcare provider long-term is important.
Good Skincare Habits Help Prevent Disorders
While avoiding problems completely can be tricky, taking good care of your skin certainly helps.
- Wash your face morning and evening with lukewarm water and a mild cleanser. Avoid harsh scrubs and pat, don’t rub, your skin dry.
- Use only oil-free and noncomedogenic makeup and remove at the end of each day.
- Read product labels so you know what ingredients are present and how they work. Trial-and-error is the best way to find out what items work best for your skin.
- If you exfoliate, do so only a few times a week to avoid the irritation that can lead to skin disorders.
- Routinely wash hair to control oil buildup that clogs pores.
- Keep hands away from your face. Despite frequent handwashing, dirt, bacteria, oil, and all manner of pollutants are always present, just waiting to irritate your skin.
It’s a good idea to understand what kinds of skin disorders can affect you—there are lots more than what we’ve covered here. Knowledge gets you prepared for whatever comes your way.

